A global view on the impact of Ebola
The outbreak caused enormous economic damage to the countries affected, led to travel restrictions, the closure of schools and many other social services, destruction of jobs and the inability of people to earn their livelihoods. The World Bank estimates that the economic impact for the three outbreak countries in 2014 alone is over $500 million in losses, about 5% of their combined Gross Domestic Product (GDP).
The fact that the disease could spread so uncontrollably in Guinea, Liberia and Sierra Leone revealed the structural and systemic weaknesses of the health systems in these countries, caused by decades of lack of investment in public sector health systems and the totally inadequate attempts at redevelopment following the end of the civil conflicts in Liberia and Sierra Leone. Moreover, these weaknesses have a direct impact on the surrounding countries and even countries much further away, with EVD infections and deaths reported in the United States and Spain.
The immediate general response to the EVD outbreak was essentially “technical” and “logistical” (mobilizing external assistance, providing resources, infrastructure etc.). However, such responses cannot address the structural and long-term political challenges of non-functioning public health systems lacking in decent working conditions and totally inadequate in providing universal coverage, let alone confronting a major health disaster.
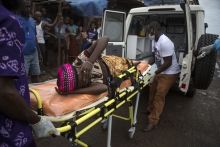
The deplorable state of the healthcare sector caused an unprecedented number of medical staff to get infected by the disease. Healthcare workers and nurses were confronted with lack of personal protective equipment (PPE), unsafe working environments, substandard infrastructure, over-exposure to hazardous environments, structural understaffing and a complete lack of sufficient resources to deal with the scale of infections.
More than 500 health workers died of Ebola due to the poor working conditions and safety measures, which only aggravated the health situation in the three most affected countries.
A study of the World Bank Group indicated that “as of May 2015, 0.11% of Liberia’s entire general population had died due to Ebola, as compared with 8.07% of its health workers, defined in the study as doctors, nurses and midwives. In Sierra Leone, the loss was 0.06% of the general population compared with 6.85% of the health workers, while 0.02% of Guinea’s overall population had died compared with 1.45% of all health workers. According to the report this translates into a 10% reduction of doctors in Liberia and an 8% reduction in nurses and midwives. In Sierra Leone, it means a 5% reduction in doctors and a 7% reduction in nurses and midwives. In Guinea, the reduction is smaller, 2% for doctors and 1% for nurses.”
To make matters worse, those fighting on the frontline were severely underpaid. Regardless of the large amounts of money directed to the three Ebola countries, health workers often went without pay and risk allowances, and were torn between fighting for their rights or fighting the disease. Furthermore, Public Services International (PSI) received reports that health workers who have died are not being covered by (already severely inadequate) social security systems and their families are left destitute.
It was striking that in the three most affected countries, Sierra Leone, Guinea and Liberia, public sector unions have been almost absent from the development of the action plans. The fact that unions can play a positive role in the elaboration of a response is nonetheless proven by Nigeria, where unions gave early warnings and ultimately government and healthcare unions worked closely together to successfully stop the spread of the disease.
The health sector unions represent the healthcare workers who are the experts on fighting Ebola and therefore have the best insights into the needs of a strong national healthcare sector. As one of them stated: “We are the ones who wear the shoe and therefore know best where it doesn’t fit”.
-
Read the publication on-line
-
Download a PDF of "PSI's Trade Union Response to the Ebola Virus Disease"
-
More on the PSI's Ebola response
-
Also see PSI's work on Health and Social care services
In this issue:
- Foreword: PSI Health Priorities and Trade Union Response to the Ebola Virus Disease
- A global view on the impact of Ebola
- Trade union response: the ebola response strategy
- Work on the ground: three national action plans
- The survey: mapping missing wages, hazard fees and family support
- Lobby: visits in the three most affected countries and the United States
- Liberia: trade union rights under attack
- Congo: unite the unions
- Ghana: unions involved

